 Learn More
Learn More Learn More
Learn More


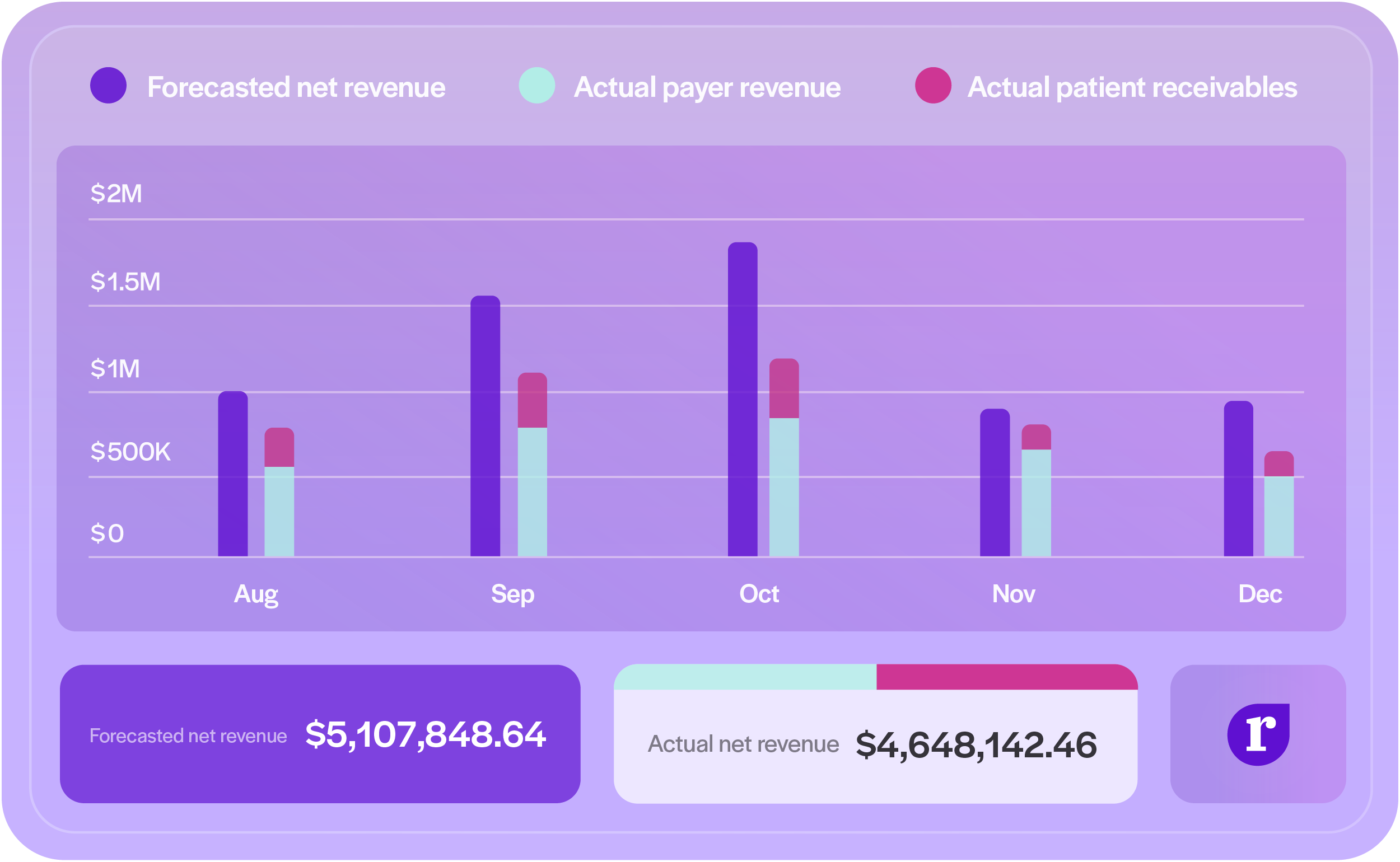
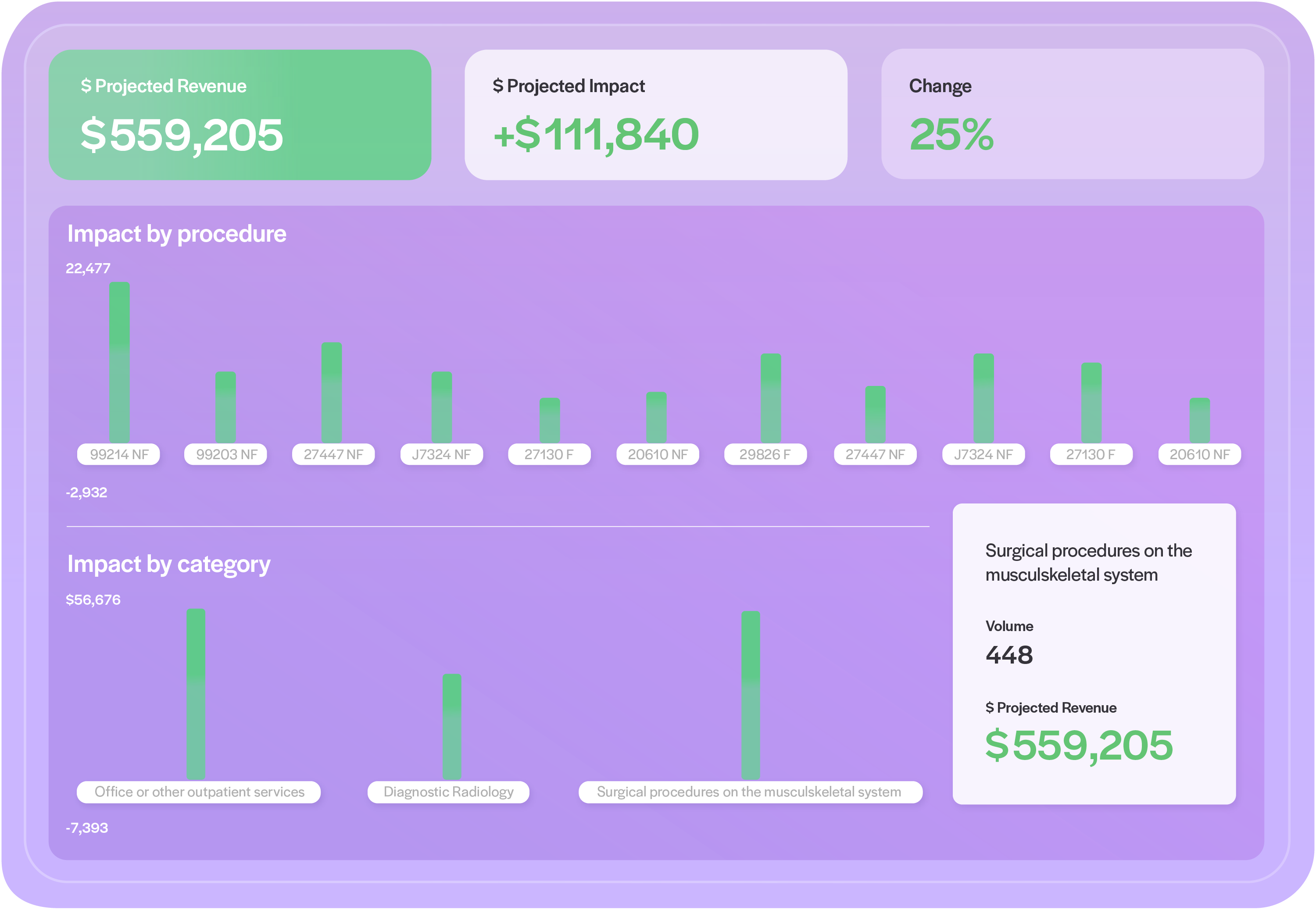

















“Medical contracting is like the biggest black box. It’s confusing on our side as the providers, and it’s confusing on the payer’s side as they adjudicate claims. There is no way to know how well your contracts are performing without a tool like Rivet. The analytics and data aggregation tools in Rivet are great: we can sort and display claims data in ways you’d never be able to do on your own. It’s awesome. Rivet’s software is a necessity to manage medical practices of any size.”
Peggy Harris
Chief Financial Officer

“We have the highest level of transparency with Rivet that we couldn’t get anywhere else. As a bonus, it’s also functional and easy to use, making it easy to gain big picture and granular insights in only a few clicks.”
Sharon Bromley
CEO

“We used to work on a contract negotiation for months, if not longer. But with Rivet, we can get negotiation preparations done so much quicker. What used to take 1-2 months can now be done in less than a week. There’s no way we could prepare for negotiations that quickly without Rivet. We currently have 2 negotiations that are going our way because of Rivet.”
Shannon Young
Business Services Director

“Rivet has driven up revenue massively. It paid for itself in less than a month. The biggest thing is that we're getting paid what we're supposed to using Rivet. ”
Jennifer Davison
Chief Executive Officer

“With Rivet, we see cost savings in automating countless manual processes, less AR days, and in detecting underpayments. Plus, their customer support makes it feel like their team is right in our office.”
Kellie Ickowski
Practice Administrator

“Now, providing estimates for even the most complicated plans is really easy. With Rivet, you can go in, pick the right carrier or plan, enter the codes they’re getting billed for, and provide an estimate.”
Stephanie Collins
Chief Executive Officer



Same appointment schedule & care. More Revenue.
Download Ebook
Learn more practical methods for predicting revenue.
Download Whitepaper
